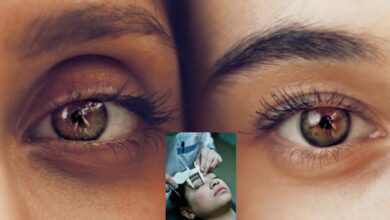
Milia, colloquially known as Milialar in Turkey, are small, pearl-like cysts that commonly manifest on the skin, particularly around the eyes and eyelids. Despite their benign nature, these tiny bumps can be a source of distress due to their distinctive appearance. This comprehensive guide aims to unravel the intricacies of Milialar, exploring its types, development process, signs and symptoms, preventive measures, and various treatment options.
Table of Contents
Understanding Milia:
Milia are characterized by small, dome-shaped bumps ranging from 1-2 millimeters, resembling pinheads. Their whitish-yellow, pearly appearance gives them a distinct texture on the skin, often likened to tiny pearls embedded beneath the surface. While these bumps are commonly associated with newborns, adults can also develop Milialar, frequently as a result of skin damage.
Types of Milia:
Milialar can be categorized into two primary types: Primary Milia and Secondary Milia.
Primary Milia.
– Directly formed as a result of keratin entrapment within the skin.
– More commonly observed in neonates due to immature sweat ducts.
-Small, white to yellow cysts, usually asymptomatic, are frequently found on the face, particularly around the eyes, nose, and cheeks.
-They frequently resolve on their own in infants within weeks to months.
Secondary Milia:
– Arises as a result of trauma or injury to the skin.
– Occurs in adults after specific skin conditions or procedures.
– Similar appearance to primary Milia, often seen in areas where an injury or procedure occurred.
– Duration varies and can last for a long time depending on the cause.
– Treatment involves addressing the underlying cause, with options like manual extraction, laser therapy, or medications.
What Causes Milia or Milialar Development?
Milia formation is intricately linked to the entrapment of dead skin cells beneath the skin’s surface, resulting in the formation of tiny cysts. While they commonly appear on the face, particularly around the eyes and cheeks, Milialar can also manifest elsewhere on the body. Several contributing factors include:
Genetics.
– Some individuals have a hereditary predisposition for developing Milia, often running in families.
Sun Exposure.
– Prolonged exposure to the sun can damage facial skin over time, increasing the risk of Milia.
Skin Trauma.
– Injuries such as cuts, burns, abrasions, and blisters may lead to Milia during the healing process.
Medical Conditions.
– Disorders causing dry skin and inflammation, such as eczema, can elevate the risk.
Medications.
– Certain medications, like steroids, may promote Milia as a side effect.
Heavy Creams and Makeup.
– The use of thick, greasy products can clog pores and contribute to cyst formation.
Milia is most commonly observed in newborns, with up to 50 percent of infants experiencing transient Milia that typically resolves within a few weeks. Maternal hormones are believed to play a role in this occurrence. However, persistent Milialar affects approximately 2.5% of the general adult population, with women more frequently affected than men. The prevalence of Milia tends to increase with age, attributed to age-related changes in skin cell kinetics and decreased skin elasticity.
The Development Process:
The formation of Milialar follows a specific sequence:
Skin Renewal.
– As part of its natural renewal process, the skin sheds dead cells.
Trapped Keratin.
– Sometimes, these cells fail to shed properly, leading to the formation of trapped keratin.
Formation of Cysts.
– The accumulation of keratin results in the formation of tiny cysts beneath the skin, giving rise to Milia.
Expert insights highlight several subtypes of Milialar, with primary Milia spontaneously arising due to keratin entrapment being most common around the eyelids. Secondary Milialar can result from trauma, burns, blistering, or ophthalmic conditions.
Signs and Symptoms of Milia or Milialar:
Milia are easily identifiable due to their characteristic features:
– Small, pearly white bumps on or around the eyelids.
– Under the skin, dome-shaped, smooth bumps that resemble pearls.
– Whitish-yellow or yellowish-white in color.
– May appear singly or in clusters.
– They are usually painless and do not itch or irritate the skin.
– In some cases, Milia may secrete a waxy, cheese-like discharge if ruptured.
-They can last for weeks or months before disintegrating.
If uncertainty or concerns about any skin condition arise, consulting a dermatologist for a proper diagnosis and guidance is advisable.
Preventive Measures:
While complete prevention of Milialar may be challenging, adopting certain practices can help reduce the risk:
– Use oil-free, non-comedogenic moisturizers and makeup.
– Keep heavy, greasy creams and cosmetics away from your eyes.
– To unclog pores, cleanse gently and exfoliate on a regular basis.
– Shave carefully using proper technique to avoid skin injuries.
– Wear sunscreen daily and limit unprotected sun exposure.
– Keep the skin well-hydrated to prevent excess dryness.
– Thoroughly remove makeup before bedtime and discard old products.
– Address any underlying skin conditions, such as eczema.
– If you are prone to Milia, avoid intensive facials or chemical peels.
Treatment Options for Milia:
In most instances, Milia resolves spontaneously within weeks to months and may not require treatment. However, if the bumps persist or cause distress, various treatment options are available:
- Prescription Retinoid Creams
- Microdermabrasion
- Chemical Peels
- Electrocautery
- Manual Extraction
- Cryotherapy
- Laser Ablation
- Surgical Removal
It’s crucial to note that this information is provided for educational purposes, and seeking professional advice from a dermatologist before pursuing any treatment is recommended.
Conclusion:
In conclusion, Milialar, the small pearl-like cysts that can appear on the skin, are generally harmless and can be found on the eyelids and around the eyes. While they are more common in newborns, adults can also develop them, often as a result of skin damage or trauma. Milia comes in different types, each with its own characteristics and development processes. Despite their benign nature, the appearance of Milia can be a cause for concern, prompting individuals to seek guidance on preventive measures and available treatments.
Visit for more best articles